Neck Pain Exercises: The Physiotherapist’s Guide to Fixing It Yourself
Written by Stuart Maytham, BSc Physiotherapy, HCPC Registered | Last reviewed April 2026
This is the same advice our physiotherapists in Edinburgh give in clinic every day. We’ve put it here for free because the best outcomes happen when people understand their pain, not just follow a list of exercises.
In this guide you’ll find the neck pain exercises that actually work, backed by evidence and tested with hundreds of patients, plus what’s causing your pain, which type you have, and the five myths keeping you stuck.
Created by qualified physiotherapists. No sign-up required.
What causes neck pain?
Neck pain is almost always caused by increased sensitivity in the nervous system rather than structural damage. Understanding this is the single most useful thing you can do before you start any exercises.
The most common triggers are a combination of lifestyle factors: poor sleep, stress, reduced physical activity, and prolonged static positions. You don’t need an injury or tissue damage for your neck to feel genuinely sore and restricted.
Less commonly, neck pain can involve nerve irritation or age-related joint changes. Even in those cases the same principles of movement and load management apply. We cover the different types in detail below.
When should you seek medical attention?
Most neck pain is not serious and will improve with the right approach. However, seek urgent medical attention from your GP, NHS 111, or A&E as appropriate if you have any of the following:
- History of cancer
- Fever or signs of infection
- Sudden severe pain following a fall or impact
- Neck stiffness combined with difficulty lifting both arms overhead
- Pain, tingling, numbness or weakness into your arms or legs
- History of inflammatory disease, particularly if you are on immunosuppressants
- You are under 18 or over 55 with a new onset of symptoms
No red flags? The rest of this guide is for you.
Why does your neck hurt? Understanding pain before you exercise
Neck pain is almost always caused by increased sensitivity in the nervous system rather than structural damage. Understanding this is the single most useful thing you can do before you start any exercises.
Pain is your brain’s alarm system. It fires when your brain judges a situation to be threatening, but just like a smoke alarm can trigger when there is no fire, you can have real, significant pain with no tissue damage at all.
Two examples that make this clear. Phantom limb pain, where someone feels intense pain in a limb that no longer exists. And the opposite: soldiers in combat who sustain serious injuries but feel no pain until they are out of danger. Context changes everything.
The other thing people find surprising is that pain is not proportional to damage. A 2015 study found that 37% of 20-year-olds had disc changes on scan with zero pain. Your neck may be sensitive without being damaged.
Think of your body not as a machine that needs fixing, but as an orchestra. If something is not working, the goal is to retune it, not replace parts. That is what the exercises and advice in this guide are designed to do.
One more important distinction: discomfort is not the same as harm. When you start moving a painful neck, it will feel uncomfortable. That is expected and appropriate. The NHS gets hip replacement patients moving the same day as surgery, not to cause pain, but because movement is what heals.

What type of neck pain do you have?
There are three main types of neck pain. Knowing which one you have helps you understand what to expect and how to approach your recovery.
Non-specific neck pain
This is the most common type and the main focus of this guide. There is no single identifiable cause.
Instead it is a combination of lifestyle factors: poor sleep, stress, reduced physical activity, and prolonged static positions. You do not need an injury or tissue damage for your neck to feel genuinely sore and restricted.
Common signs include pain around the neck that may spread to the shoulder or base of the skull, stiffness, restricted movement, and associated headaches. The good news is that non-specific neck pain responds very well to the right exercises and lifestyle changes.
Whiplash
Caused by a sudden force, most commonly a road traffic accident, where the neck is rapidly moved beyond its normal range. This irritates muscles, joints and nerves.
Whiplash can be persistent but the evidence is clear that graded movement and activity leads to better outcomes than rest and protection.
Cervical radiculopathy
This is when a nerve root in your neck becomes compressed or irritated, often from a disc bulge or bony change at one of the spinal levels. The key distinguishing feature is symptoms travelling down your arm: pain, tingling, numbness or weakness into the hand or fingers. This type benefits from a more specific assessment and a one-to-one appointment with a physiotherapist is worthwhile if you suspect it.
5 neck pain myths that are keeping you stuck
These beliefs are extremely common and they are often what keeps people in pain longer than they need to be.
Myth 1: Your neck hurts because of bad posture
“Text neck.” “Forward head posture.” These terms get thrown around constantly but the research does not support them. Multiple studies have found that neck posture is not reliably linked to neck pain. People with so-called poor posture frequently have no pain at all, while people with textbook-perfect posture can have chronic symptoms.
One of our patients, Robert, did his rehab exercises with a noticeably rounded upper back. He was pain-free and performing all his daily tasks. Posture did not cause his pain and correcting it was not the goal.
The real issue is staying in any position for too long without moving. The worst posture is the one you hold for hours. Focus on breaking up static time every 60 to 90 minutes rather than obsessing over how you sit.
Myth 2: You should rest and protect your neck until the pain goes away
This feels logical. If it hurts, stop moving it. But beyond the first 48 to 72 hours, rest is counterproductive.
Avoiding movement causes muscles to weaken and stiffen, keeps your nervous system in a heightened state of sensitivity, and extends recovery rather than shortening it.
Gradual, progressive movement is the treatment. Not rest.
Myth 3: Your neck is out and needs cracking or manipulating
Joints do not pop in and out of place. Manipulation can give short-term relief but a systematic review of 47 randomised trials covering over 4,000 participants found that manipulation alone provides no meaningful long-term benefit for neck pain. It also creates dependency in some people where they need regular treatment just to maintain function. That is not recovery.
Myth 4: You need a neck brace
If you have seen neck braces used on TV after whiplash injuries it is understandable to think they help. They do not, at least not for most neck pain. Unless a clinician has prescribed one following serious trauma, wearing a neck brace immobilises the muscles and joints that need to move and strengthen. It also reinforces the idea that your neck is fragile and needs protecting, which is the exact belief that slows recovery.
Myth 5: Neck pain is just wear and tear and comes with age
Neck pain affects people of all ages. In a 2015 study, 37% of 20-year-olds had disc degeneration on scan with no pain. By age 80, 96% had disc changes and most were still pain-free. Disc changes are like wrinkles on the inside. They are a normal part of ageing, not an explanation for your pain and not a reason to avoid movement.
This is also why scans are rarely useful for neck pain without red flags. The finding will not change the treatment.
Myth 6: Pain medication just masks the pain
Short-term pain relief used as directed by your GP or pharmacist can actually support recovery by letting you move more comfortably. Acute neck pain is primarily about sensitivity rather than damage. Anti-inflammatories can break the cycle of pain, guarding, stiffness and more pain. If they help you get moving that is a good outcome.
Always follow your GP or pharmacist’s guidance on dosage and duration.
Not sure which of these applies to you?
A free online physiotherapy assessment gives you a clear personalised answer in one session.
How to fix neck pain: the evidence-based approach
The good news is that most neck pain responds well to simple, consistent self-management. The neck pain exercises below follow what the evidence actually supports, movement, progressive load, and consistency.
Short-term relief
If your neck is acutely painful, a few things can help in the short term. A sports massage can reduce muscle tension and sensitivity and has good evidence for improving mood and reducing stress alongside the physical benefits. Heat from a hot bath or heat pad works for similar reasons — your muscles and nervous system respond well to warmth.
These are useful tools for getting comfortable enough to move. They are not a cure and should not replace the longer-term work.
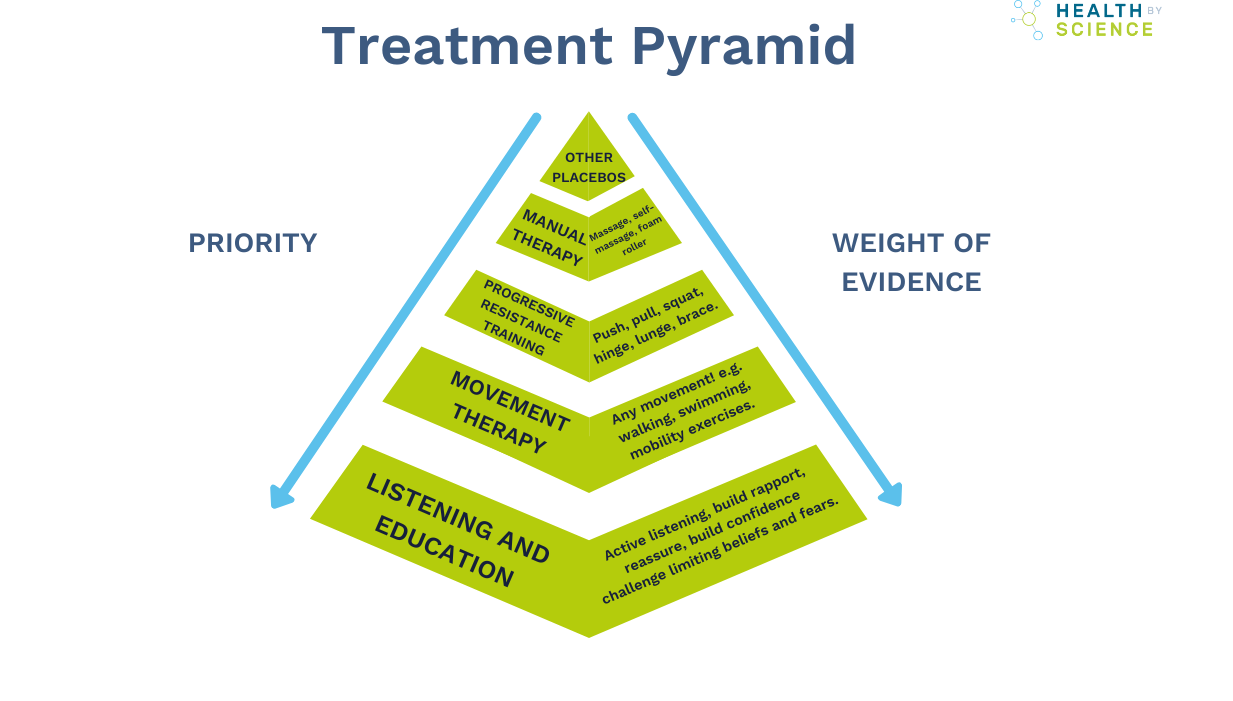
The long-term fix: movement and load
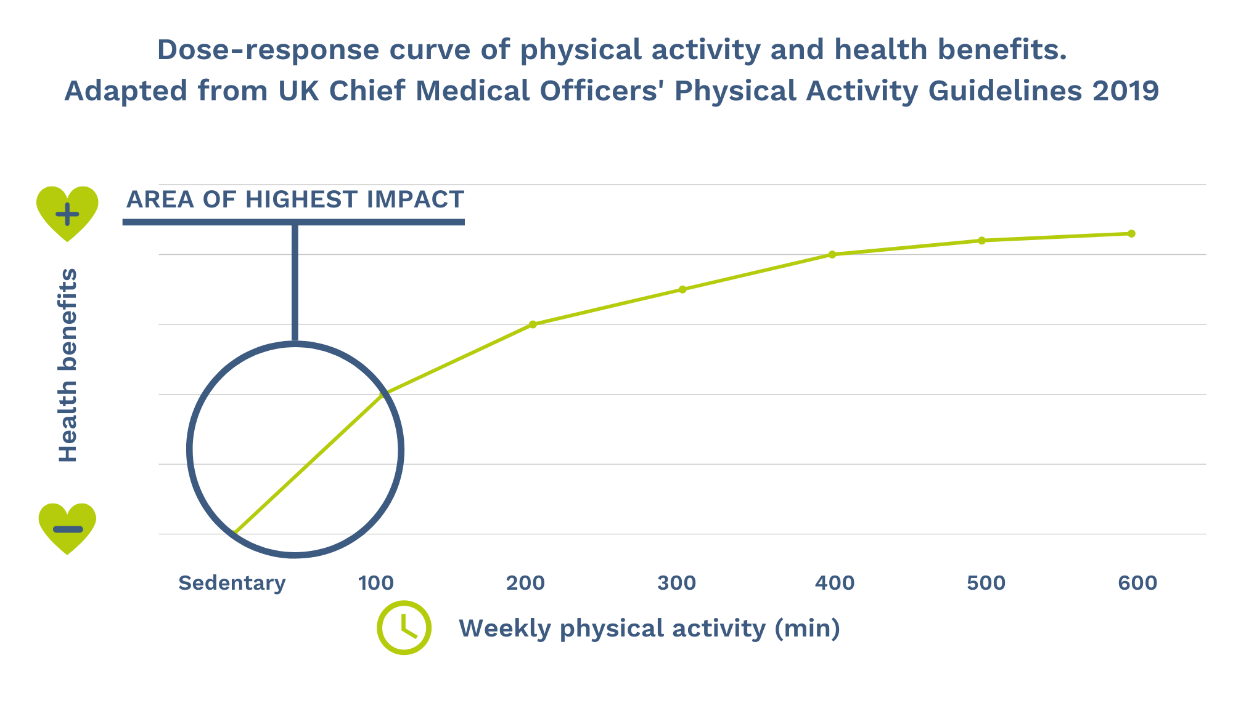
The treatment pyramid above shows where your time and effort are best placed. At the base, and with the strongest evidence, is movement therapy. Physical activity is one of the most effective painkillers available and the dose-response curve shows that the biggest gains come when you go from doing nothing to doing something. Even a 5-minute walk each day provides meaningful benefit.
Building on that foundation is progressive resistance training. Working with a personal trainer or following a structured programme strengthens the muscles of your neck and upper back, builds resilience and reduces sensitivity over time. The exercises in this guide are designed to do exactly that.
Manual therapy such as sports massage in Edinburgh can play a supporting role but works best alongside exercise rather than instead of it.
The Goldilocks principle
Too little movement and your muscles weaken and stiffen, keeping sensitivity high. Too much and you risk a flare-up that sets you back. The goal is the middle ground, movements that feel uncomfortable but tolerable, where you can breathe steadily through them.
Think of your physical capacity as a cup. The larger you build that cup through consistent movement, the more stress your neck can handle without tipping into pain.
The pyramid below shows where your time and effort are best placed, from the most impactful at the base to the least at the top.
The curve below illustrates how the greatest health gains come from the earliest increases in activity, when you go from sedentary to simply moving more.
How much should you move your neck? Rest versus exercise explained
You should start moving your neck after the first 48 to 72 hours. Beyond that point, rest makes things worse, not better.
When you move your neck through a comfortable range you create small adaptive signals that tell your brain and nervous system to become more resilient. Over time your capacity cup gets bigger and your neck can handle more without triggering pain. This is bioplasticity in action.
Finding the right level
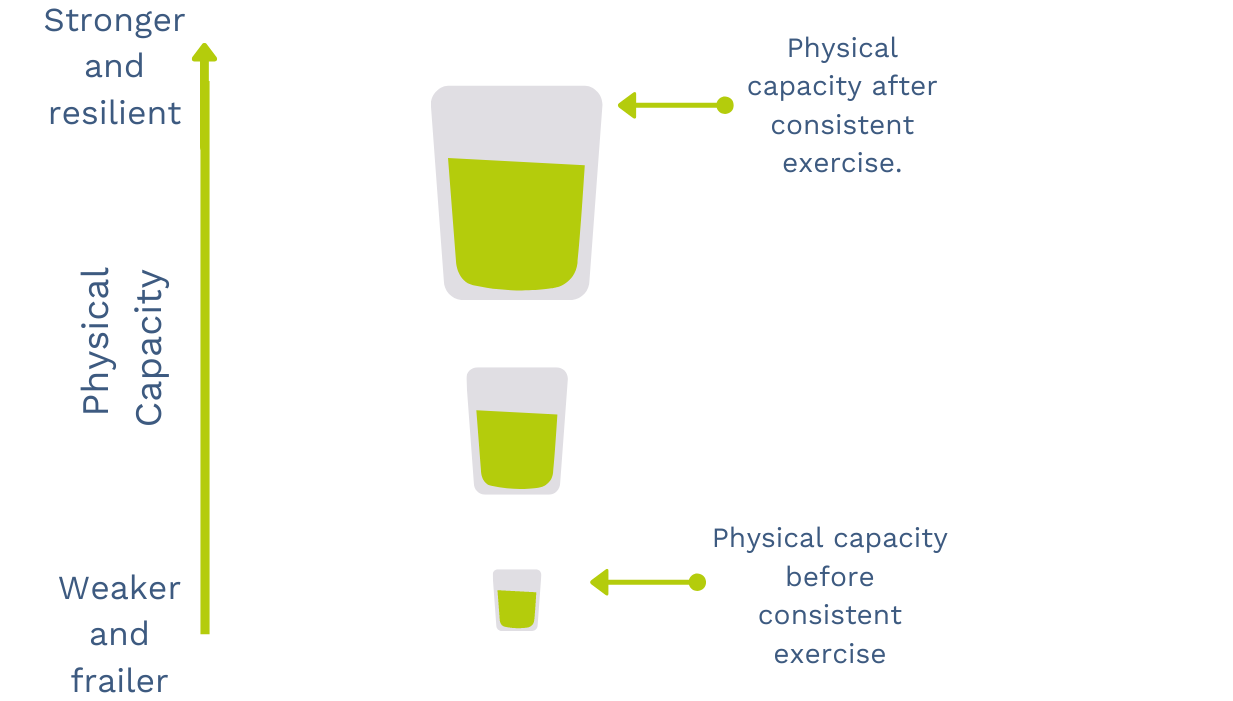
Use a 0 to 10 pain scale to guide yourself. Aim for movements that sit around a 4 to 5 out of 10. Uncomfortable but tolerable. You should be able to breathe steadily through the movement. If it hits 7 or above and you cannot breathe comfortably, reduce the range or intensity.
The optimal load graph above illustrates this clearly. Too little stress leads to deconditioning. Too much leads to a flare-up. The goal is the middle ground.
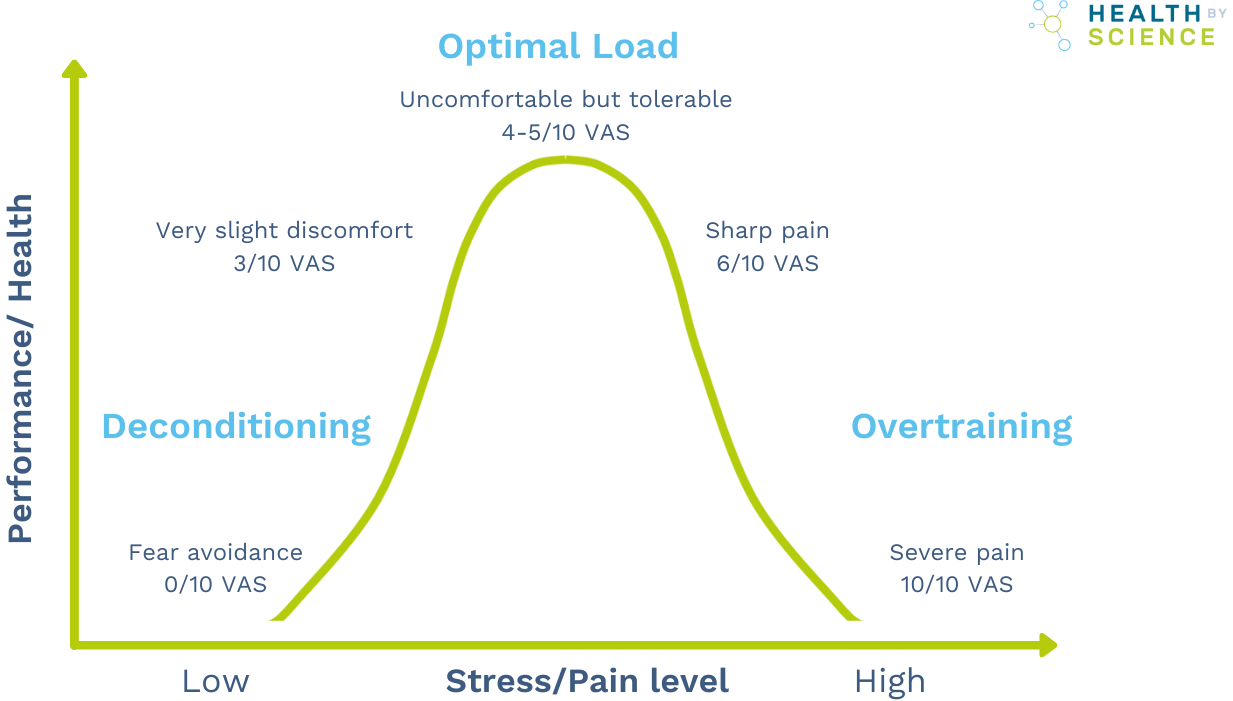
Over time your capacity cup gets bigger and your neck can handle more without triggering pain.
Recovery is part of the process
Your body adapts during rest, not during the exercise itself. Good sleep and stress management are not optional extras in your rehab, they are core to it. High mental or physical stress without adequate recovery keeps sensitivity levels elevated and slows progress.
Do the work. Recover well. Repeat consistently.
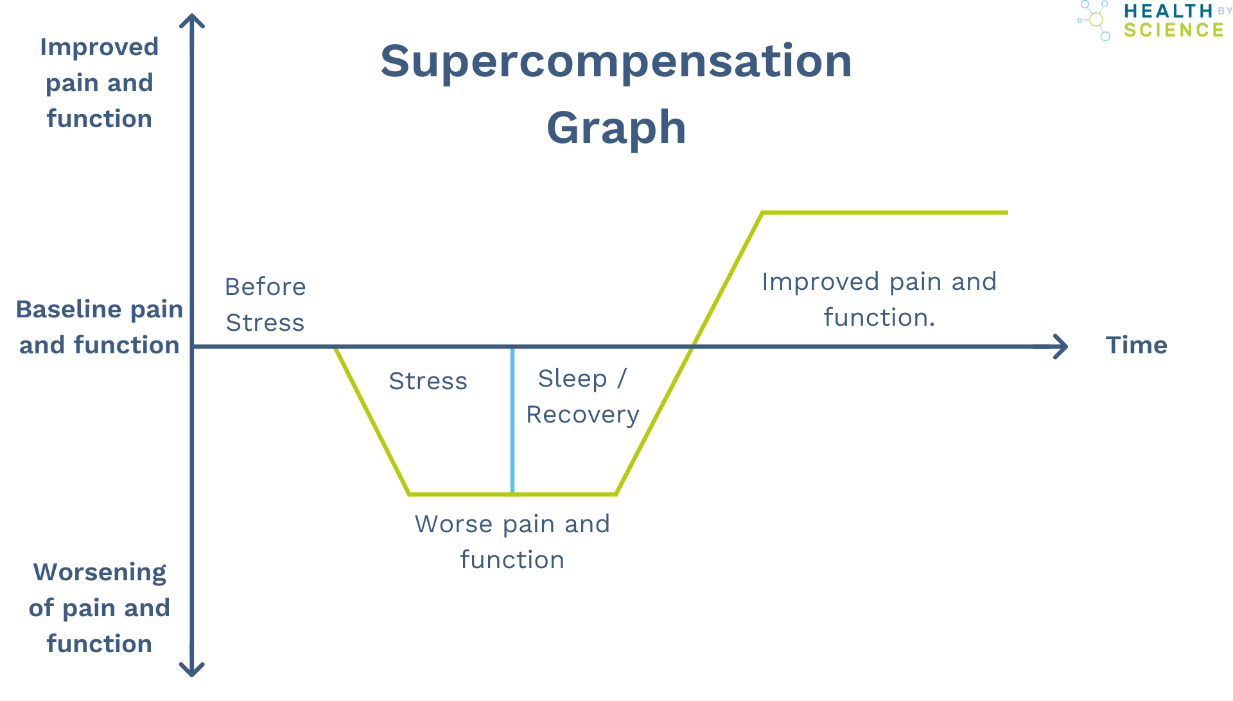
The supercompensation graph below shows how stress followed by adequate recovery leads to improvement over time.
Not sure which of these applies to you?
A free online physiotherapy assessment gives you a clear personalised answer in one session.
How long does neck pain take to heal?
Most neck pain improves significantly with consistent neck pain exercises, but recovery is rarely a straight line. Understanding what to expect helps you stay on track when you have a difficult day.
Tissue healing timeframes
Different structures heal at different rates. Muscles typically settle within 4 to 6 weeks with consistent movement and load. Tendons and ligaments take longer, usually around 12 weeks to remodel and regain full load tolerance.
That does not mean you will be in pain for the entire duration. Most people notice meaningful improvement within the first few weeks. The timeframes above reflect when tissues are genuinely robust again rather than just comfortable.
Progress is not linear
A bad day does not mean you are going backwards. It usually means you have had poor sleep, a stressful week, or pushed slightly too hard. Zoom out and track weekly trends rather than daily symptoms.

Tissue healing timeframes
Rather than aiming to be better by a specific date, work through these stages at your own pace:
- Pain settling — moving with less sensitivity
- Range of movement improving — turning your head freely
- Strength returning — neck feeling stable and resilient
- Full return to normal activity — no limitations
When to get help
If you have been doing the right things consistently for 6 weeks or more and are not seeing meaningful progress, a one-to-one assessment with one of our physiotherapists is the right next step. There may be something more specific going on that needs a clinical eye.
The best neck pain exercises
These exercises have been chosen based on the best available research and our clinical experience treating neck pain. They are the same exercises we prescribe most often in clinic.
The most effective exercises are usually the ones that feel challenging and slightly uncomfortable. That is a sign you are working in the right range. Aim to do these at least twice a day, starting with 5 repetitions and building up to 15 as you feel able.
Use the 0 to 10 pain scale to guide yourself. Working at a 4 to 5 out of 10 is the goal. If it exceeds 6 out of 10 ease off. Breathe out as you move into discomfort — this helps your nervous system relax into the movement.
Want a printable version to take to the gym or follow at home? Download the free PDF below.
Exercise 1: Neck Isometrics
Isometrics are the best neck pain exercises to start with. They strengthen your neck muscles without moving your head, making them safe and effective in the early stages when movement feels sensitive.
How to do it:
Sit or stand tall with your head in a neutral position. Place your hand against your head and gently push your head into your hand, creating resistance. Do not allow your head to move. Hold for 5 seconds then release.
Perform in four directions:
- Flexion: palm on forehead, push forward
- Extension: palm on back of head, push backwards
- Left rotation: palm on left cheek, push left
- Right rotation: palm on right cheek, push right
- Left side flexion: palm on left temple, push left
- Right side flexion: palm on right temple, push right
Sets and reps: 1 sets of 5 to 15 repetitions in each direction, twice daily. Build to 15 reps as you feel able.
What to feel: Mild muscle fatigue and tension in the neck. Breathe steadily throughout. If you feel sharp pain or symptoms radiating into your arm, ease off and consult a physiotherapist.
That does not mean you will be in pain for the entire duration. Most people notice meaningful improvement within the first few weeks. The timeframes above reflect when tissues are genuinely robust again rather than just comfortable.
Exercise 2: Active Neck Range of Movement
Once isometrics feel manageable, active range of movement neck pain exercises help restore full, pain-free motion. These work by gradually desensitising the nervous system and improving mobility through the full arc of movement.
How to do it:
Sit or stand tall. Move slowly and with control through each direction, breathing out as you move into discomfort. Do not force range — work to your comfortable limit and aim to increase it gradually over time.
Perform in four directions:
- Flexion: chin slowly down towards chest
- Extension: head slowly back, eyes to ceiling
- Rotation: turn head slowly left then right
- Side flexion: ear slowly towards shoulder left then right
Sets and reps: 1 sets of 5 to 15 repetitions in each direction, twice daily. Build to 15 reps as you feel able.
What to feel: A comfortable stretch and mild discomfort at end range.
This should ease as you repeat the movement. If symptoms are significantly worse after, you have done too much — reduce the range next time.
Exercise 3: Wall Angels
Wall angels are a slightly different type of neck pain exercise, they target the upper back and shoulders that support your neck, rather than the neck directly. Weakness in this area is one of the most common contributing factors to persistent neck pain and is often overlooked.
How to do it:
Stand with your back flat against a wall, feet a few centimetres away from the base. Press your lower back, upper back and head gently into the wall. Bring your arms up to the wall with elbows bent at 90 degrees, like a goalpost position. Slowly slide your arms up the wall above your head, keeping contact with the wall throughout, then slide back down to the start position.
Sets and reps: 2 sets of 5 to 10 repetitions, twice daily. Build to 15 reps as you feel able.
What to feel: Effort across your upper back and shoulders. It is common to find it difficult to keep your arms and back in contact with the wall initially, work within whatever range you can manage and it will improve with consistency.
When should you seek further help?
If these neck pain exercises haven’t produced improvement after 6 weeks or more and are not seeing meaningful progress, it is time to get a professional assessment. There may be something more specific going on that needs a clinical eye.
Our online physiotherapy assessment is a good starting point. One session gives you a clear, personalised plan based on your specific symptoms, history and goals. It is free and there is no obligation to book further sessions.
If you would prefer to be seen in person, our physiotherapy team in Edinburgh works with people at all stages of neck pain recovery, from acute flare-ups to long-standing persistent symptoms.
Not improving on your own?
Get a free online physiotherapy assessment from one of our qualified physiotherapists. One session, no obligation, clear plan.